The gut-brain axis—the two-way communication between your digestive tract and your brain—has become a major focus of nutrition and mental health research. Gut bacteria produce and respond to neurotransmitters and inflammatory signals that can influence mood, stress resilience, and emotional balance. As a certified nutritionist, I see growing interest in whether probiotics can support mental wellbeing. This article explains the science behind the mood–gut connection, what the evidence actually shows for probiotics and mood or anxiety, how to choose strains and doses, and the important limitations and practical takeaways. Probiotics are not a substitute for mental health care, sleep, or diet; they may be one useful piece of a broader approach when used evidence-based. You can compare probiotics on iHerb for strain options.
The Gut-Brain Axis: The Science
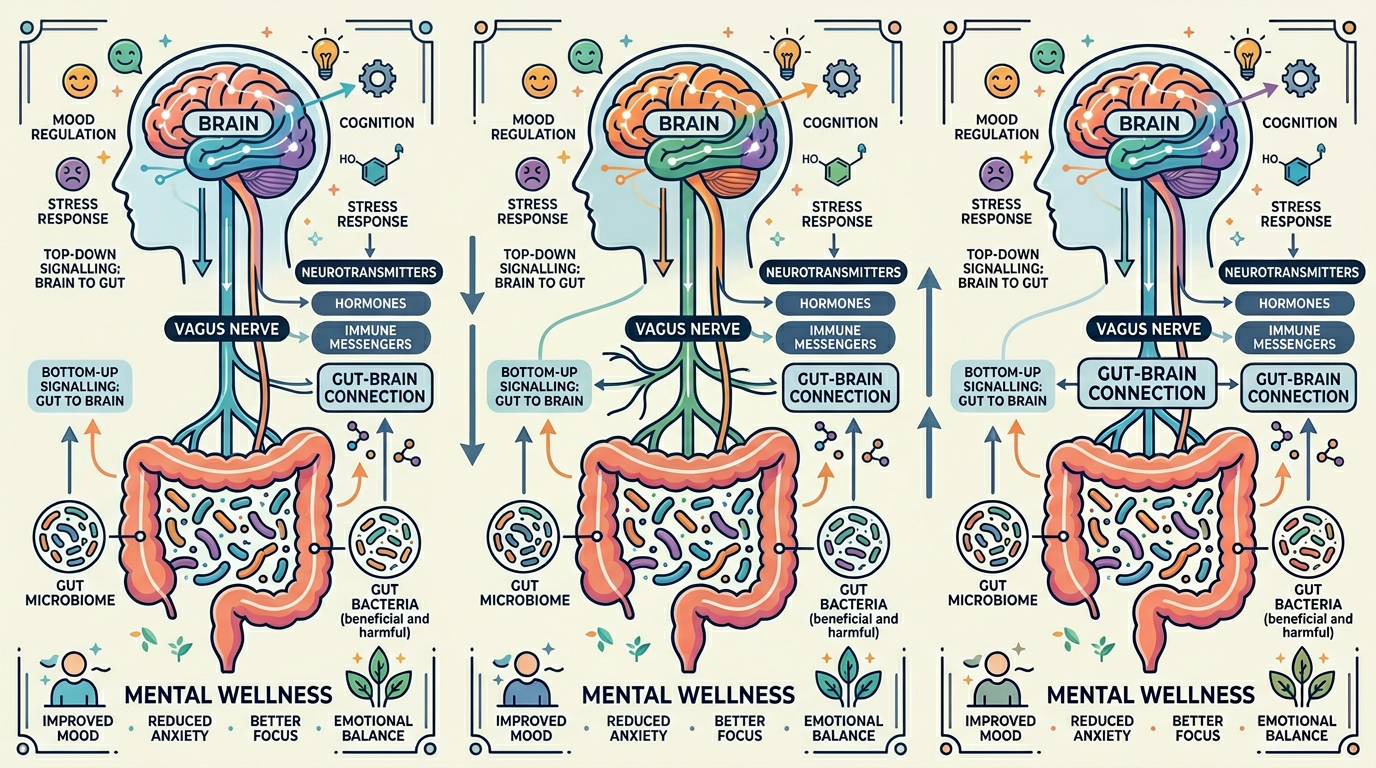
The gut-brain axis refers to the continuous, bidirectional communication between the central nervous system and the enteric nervous system in the gut. This communication happens through several pathways: the vagus nerve (which carries signals from the gut to the brain and back), the immune system (gut microbes influence inflammatory cytokines that can cross into the brain or affect behaviour), and the production of neuroactive compounds by gut bacteria. Your gut harbours trillions of microbes that can produce or modify molecules such as serotonin (much of the body’s serotonin is made in the gut), gamma-aminobutyric acid (GABA), dopamine, and short-chain fatty acids like butyrate—all of which can influence brain function and mood. Dysbiosis—an imbalance in the gut microbiome—has been associated in observational and some interventional studies with low mood, anxiety, and stress reactivity, though cause and effect are not fully established. Understanding this biology helps set realistic expectations: supporting gut health may support emotional resilience for some people, but probiotics alone do not treat depression or anxiety.
The vagus nerve is one of the main conduits: it relays information about gut contents, inflammation, and microbial metabolites to the brainstem and higher centres, and can influence stress responses and mood. In animal studies, cutting the vagus nerve sometimes abolishes the behavioural effects of certain probiotic strains, suggesting that at least part of the effect is mediated through this pathway. In humans, direct evidence is harder to obtain, but the anatomy and physiology support that gut-to-brain signalling is real. Similarly, gut bacteria can affect the immune system: they help train immune cells and influence the release of cytokines. Some of these cytokines can cross the blood–brain barrier or trigger brain responses that affect mood and fatigue. A diet and lifestyle that support a diverse, stable microbiome may therefore support both gut and brain health; probiotics are one tool within that broader approach.
Evidence on Probiotics, Mood, Stress, and Anxiety
Human trials on probiotics and mood have increased over the past decade. Meta-analyses and systematic reviews generally report small to modest effects that vary by strain, dose, duration, and population. For example, some meta-analyses suggest that certain probiotic formulations may improve subjective stress or mood scores in healthy or mildly stressed adults, while others find no significant effect. Results are mixed in clinical anxiety or depression; probiotics are not recommended as a first-line or standalone treatment. Studies often use specific strains (e.g. Lactobacillus helveticus R0052 and Bifidobacterium longum R0175 in combination) at doses of about 3–10 billion CFU daily for four to eight weeks or longer. Generalising from one product or population to everyone is not justified—individual response varies, and many trials are short-term or use different outcome measures. Overall, the evidence supports that some well-studied strains may offer a modest benefit for stress or mood in some people when used as part of a broader approach; they do not replace therapy, medication, or lifestyle foundations like sleep and diet.
In stress and anxiety, several randomised controlled trials have used the combination of L. helveticus R0052 and B. longum R0175 and reported improvements in self-reported stress, anxiety, or mood in healthy volunteers or in people with mild to moderate stress. Effect sizes are typically small; not every study replicates the finding, and baseline gut health and diet may influence who benefits. For depression, the picture is even more cautious: some meta-analyses show a small overall effect of probiotics on depressive symptoms, but heterogeneity is high and many studies are in people with comorbid digestive or other conditions. Probiotics should never be used instead of antidepressants or psychotherapy when those are indicated. The takeaway is evidence-based but cautious: probiotics may be a reasonable adjunct for general stress or mood support in some individuals, with the understanding that benefits are modest and not guaranteed.
How Probiotics May Influence Mood: Mechanisms
Several mechanisms may explain how probiotics could affect mood and stress. First, gut bacteria produce short-chain fatty acids (SCFAs) such as butyrate, which support gut barrier integrity and may reduce systemic inflammation; chronic low-grade inflammation has been linked to low mood in some research. Second, certain bacteria can produce or influence neurotransmitters: for instance, some strains may increase availability of precursors for serotonin or produce GABA. Third, the vagus nerve can be modulated by gut microbes and their metabolites, affecting brain signalling. Fourth, probiotics may help restore a more balanced microbiome after stress, poor diet, or antibiotic use—and a more diverse, stable microbiome is often associated with better mental health markers in observational studies. These mechanisms are supported by animal and in vitro work; in humans, direct proof that probiotics “cause” mood improvement is still limited. Probiotics are best viewed as one potential way to support a healthier gut environment that may, in turn, support mood—not as a direct “mood pill.”
Butyrate and other SCFAs are produced when gut bacteria ferment dietary fibre. They nourish the cells lining the colon, help maintain a tight gut barrier (reducing “leaky gut” and systemic inflammation), and may influence brain function through blood and neural pathways. Low butyrate production or a less diverse microbiome has been linked in some studies to higher inflammatory markers and poorer mood. Probiotics that increase SCFA-producing bacteria or that themselves produce beneficial metabolites could, in theory, support this axis. Similarly, the gut is a major site of serotonin production; gut microbes can affect the availability of tryptophan (a serotonin precursor) and other compounds that cross into the brain or affect the gut–brain dialogue. Again, translating these mechanisms into predictable mood benefits in humans remains a focus of ongoing research.

Strain Selection
Strain matters: not all probiotics have been studied for mood or stress, and effects are strain-specific. The most researched strains for mood and stress include Lactobacillus helveticus R0052 and Bifidobacterium longum R0175 (often sold together as a “psychobiotic” combination), Lactobacillus rhamnosus GG (studied in some anxiety and gut-brain contexts), and certain other Lactobacillus and Bifidobacterium species. When choosing a product, look for the full strain designation on the label (genus, species, and strain code). Avoid products that list only “Lactobacillus” or “probiotic blend” without strain details—you cannot assume they will behave like the studied strains. Prefer brands that disclose CFU count at expiry (not just at manufacture) and that have been used in published human trials when possible. Multi-strain products may be fine if the strains are identified and at least some have mood- or stress-related evidence; single-strain or well-defined combinations with human data are often preferable to poorly characterised blends.
Product quality varies: choose supplements from reputable manufacturers that use third-party testing or that publish stability data. Storage matters—some products require refrigeration to maintain viable counts until expiry. If you are unsure which product to try, a dietitian or pharmacist can help you match a product to the doses and strains used in the research you care about. Fermented foods (yoghurt, kefir, kimchi, sauerkraut) provide live bacteria and can support gut diversity, but they rarely specify strain or CFU; they are a useful dietary addition but not a substitute for a targeted supplement when you want a specific, studied strain for mood or stress.
Dosing and Timing
Typical studies use about 1–10 billion CFU per day, often in the range of 3–10 billion CFU, for at least four to eight weeks. There is no single “best” dose—follow the dose used in the research for the strain you choose, or the manufacturer’s instructions if the product is similar to a studied formulation. Taking probiotics consistently (daily) with a meal can improve survival through stomach acid; timing (morning or evening) is flexible unless the label specifies otherwise. Do not expect immediate results; give at least four to six weeks of consistent use to assess whether you notice any benefit. Higher doses are not necessarily better and may increase the chance of transient digestive side effects; start at the studied or recommended dose. If you take antibiotics, spacing the probiotic a few hours apart may help survival of the bacteria; continue the probiotic during and briefly after the course if your doctor agrees.
Limitations and Safety
Probiotics are not a treatment for depression, anxiety disorders, or other mental health conditions. Anyone with persistent low mood, anxiety, or thoughts of self-harm should be under the care of a doctor or mental health professional; do not replace prescribed medication or therapy with probiotics. Evidence for mood benefits is still evolving: effects are often modest, not everyone responds, and long-term data are limited. Probiotics are generally well tolerated, but some people experience gas, bloating, or digestive adjustment initially; these often resolve. In people who are severely immunocompromised (e.g. after transplant or during chemotherapy), live probiotics may carry a small infection risk—use only with medical approval. Report any worsening mood or new symptoms to your provider. Quality and labelling vary; choose reputable brands that specify strain and CFU at expiry.
If you notice no benefit after six to eight weeks of consistent use, it is reasonable to try a different strain or to focus on other levers (sleep, diet, stress management, professional support) rather than continuing indefinitely without effect. Do not stop prescribed mental health medication in favour of probiotics. If you have a history of endocarditis, central venous catheters, or severe acute pancreatitis, discuss probiotic use with your doctor before starting. Children, pregnant or breastfeeding women, and people with complex medical histories should also seek guidance. A pragmatic approach: use evidence-based strains at studied doses as a complement to lifestyle and professional care, and reassess with your provider periodically.
Practical Takeaways
Use probiotics as part of a broader approach: prioritise sleep, a varied diet rich in fibre and fermented foods where tolerated, stress management (e.g. exercise, mindfulness, social connection), and professional care when needed. If you try a probiotic for mood or stress, choose a well-studied strain and dose, use it consistently for at least several weeks, and pair it with lifestyle habits that support gut and brain health. Do not expect probiotics to replace therapy or medication. Track how you feel and discuss with your doctor or dietitian; they can help you decide whether to continue, switch strains, or focus on other interventions. A registered dietitian can align probiotic use with your overall nutrition and health goals.
Diet and lifestyle form the foundation: a fibre-rich, varied diet supports a diverse microbiome; sleep deprivation and chronic stress can worsen gut function and mood; and physical activity is associated with better gut diversity and mental wellbeing in observational studies. Limiting ultra-processed foods and excess sugar may help maintain a more favourable gut environment. If you are in therapy or on medication for anxiety or depression, discuss adding a probiotic with your provider so it can be part of a coordinated plan. Practical takeaway: probiotics may offer a small, evidence-based piece of the puzzle when used alongside these foundations—not in place of them.
Summary
- The gut-brain axis links the microbiome to mood via nerves, immune signals, and neuroactive compounds.
- Evidence on probiotics and mood is mixed; benefits may be modest and strain-dependent.
- Mechanisms include SCFAs, neurotransmitter production, vagal signalling, and microbiome balance.
- Choose strains with human evidence (e.g. L. helveticus R0052, B. longum R0175) and clear labelling.
- Typical dosing: 1–10 billion CFU daily for several weeks, with food; give 4–8 weeks to assess benefit.
- Probiotics do not replace mental health care; report worsening mood to your provider.
- Combine with sleep, diet, stress management, and professional support for best results.
Probiotics may offer a small, evidence-based piece of the puzzle for mood and stress when used alongside lifestyle and professional support. For product options, see probiotics on iHerb.