
As we age, the gut microbiome—the community of bacteria, viruses, and fungi living in the digestive tract—undergoes measurable changes that can affect digestion, immunity, and nutrient absorption. Many older adults and their caregivers wonder whether probiotics can help. The short answer is that evidence supports a role for certain strains in digestive comfort, immune support, and nutrient availability, but strain choice, formulation, medication interactions, and safety considerations matter. This guide summarizes age-related changes in the gut, what the research shows for probiotics in older adults, how to choose and use them safely, and when to favour food or supplements. For product options, you can browse probiotics on iHerb.
As a certified nutritionist, I emphasise that probiotics are not a substitute for a balanced diet, adequate fluid intake, or medical treatment. They work best as part of a broader approach that includes fibre-rich foods, regular physical activity where possible, and open communication with your doctor or pharmacist, especially when you take several medications or have a history of immune compromise or recent surgery.
Age-related changes in the gut microbiome
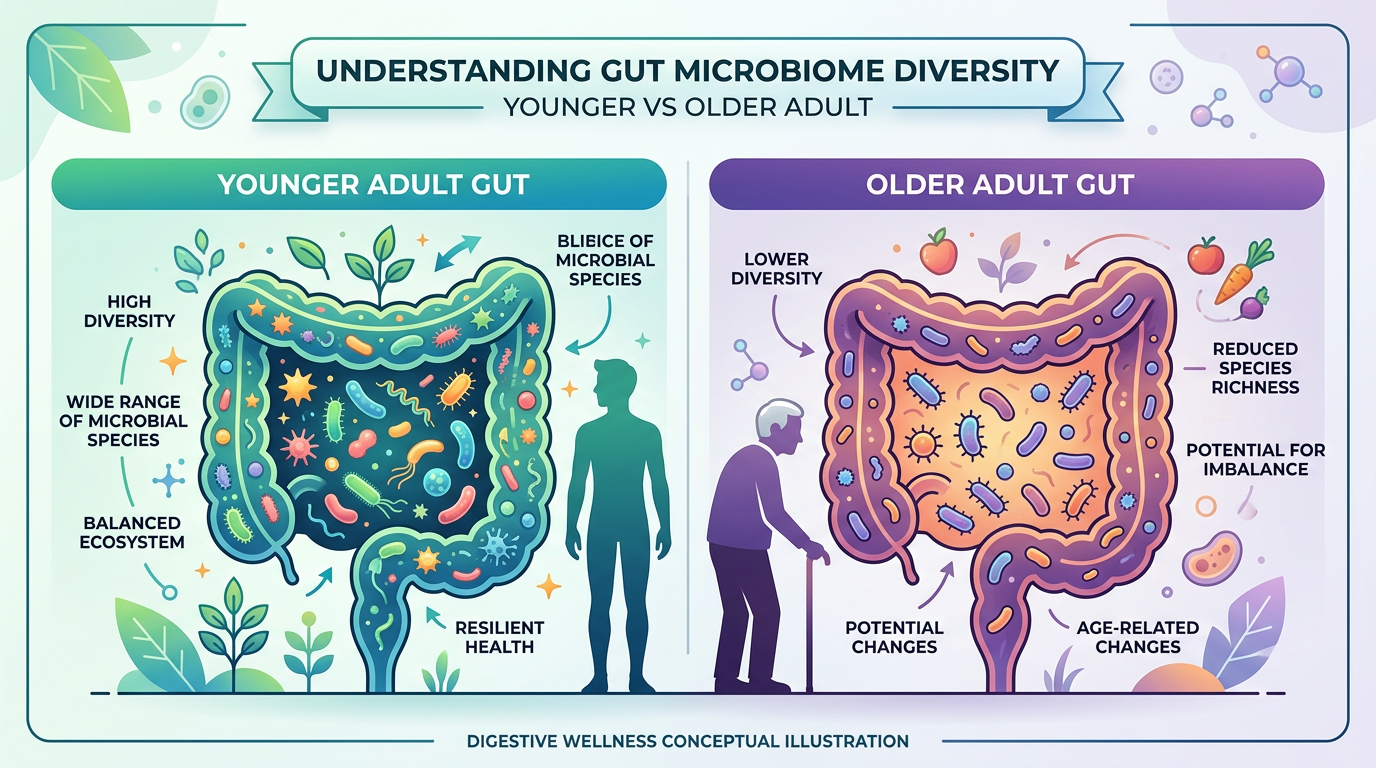
Studies consistently show that gut microbiome diversity and stability tend to decline with age. Older adults often have lower abundance of beneficial species such as Bifidobacterium and some Lactobacillus species, and shifts in the ratio of different bacterial groups. Factors that contribute include diet (e.g. limited variety, lower fibre intake, or reduced appetite), polypharmacy (multiple medications, including antibiotics and proton-pump inhibitors that can alter gut pH and microbiota), reduced mobility, hospitalisations, and surgery. Repeated or prolonged antibiotic use is a major driver of microbiome disruption; proton-pump inhibitors may reduce stomach acidity and change which bacteria survive passage to the intestine. A less diverse microbiome has been linked to poorer digestive tolerance, weaker immune responses, and in some studies to lower absorption or production of certain vitamins (e.g. B vitamins, vitamin K) and short-chain fatty acids that support gut barrier health. Understanding that these shifts are common and often modifiable helps explain why targeted support—including evidence-based use of probiotics—may be relevant for some older adults.
Evidence for probiotics in older adults
Research in older adults has grown over the past decade. While not every study shows benefit—results depend on strain, dose, duration, and population—systematic reviews and meta-analyses suggest that well-chosen probiotics can support digestive comfort, immune function, and aspects of nutrient availability when used alongside a balanced diet and medical care. The sections below summarise the main areas of evidence.
Digestion and regularity
Several randomised trials and meta-analyses in older populations suggest that specific probiotic strains can improve digestive comfort and bowel habits. Benefits may include reduced bloating, better stool frequency and consistency (e.g. in constipation-predominant settings), and fewer digestive complaints. Effects are often modest and strain-dependent; not every product or strain has been studied in seniors. Bifidobacterium lactis, B. longum, Lactobacillus rhamnosus GG, and L. acidophilus are among the most studied in ageing or older-adult populations. Consistency matters: many trials run for 4–8 weeks or longer, and benefits may not appear immediately. If you try a probiotic for digestive symptoms, give it a fair trial before switching products; initial mild gas or adjustment is common and often resolves.
Immunity
Ageing is associated with immunosenescence—a gradual decline in immune function—and the gut microbiome helps shape immune responses. Some trials in older adults report that certain probiotics (e.g. Lactobacillus and Bifidobacterium strains) can modestly improve markers of immune function or reduce the incidence or duration of upper respiratory infections. Results vary by strain, dose, and population; probiotics are not a substitute for vaccination, good nutrition, or medical care, but they may offer supportive benefit when chosen and used appropriately. Anyone with significant immune compromise (e.g. recent transplant, chemotherapy, or immunosuppressant therapy) should use live probiotics only under medical supervision.
Nutrient absorption
The gut microbiota is involved in producing or influencing the availability of some vitamins (e.g. B vitamins, vitamin K) and short-chain fatty acids that support gut barrier and metabolic health. In older adults with reduced diversity or after antibiotic use, probiotics may help restore a more favourable environment for nutrient absorption and microbial metabolism. Evidence is still evolving; probiotics should complement, not replace, a balanced diet and treatment of deficiencies when identified by a clinician. If you have known deficiencies (e.g. B12, vitamin D), follow your provider’s treatment plan and use probiotics as an adjunct where appropriate.
Strain and formulation considerations

Not all probiotics are alike. Strain identity, dose (often given in colony-forming units, CFU), formulation (capsules, sachets, drops, or foods), and storage conditions affect survival and potential benefit. For older adults, prefer products that list the full strain name (e.g. Lactobacillus rhamnosus GG, Bifidobacterium longum BB536), provide a CFU count at expiry (not just at manufacture), and have been studied in ageing or senior populations when possible. Multi-strain products may offer broader support but are not always better; single-strain or well-defined multi-strain combinations with human data are preferable to poorly characterised blends. Enteric-coated or delayed-release formulations can improve survival through stomach acid, which may be relevant for some users. Check whether the product requires refrigeration; stability at room temperature can be convenient for travel or for those who might forget to refrigerate.
Liquid and sachet forms can be easier for anyone who has difficulty swallowing capsules; follow label instructions for mixing and dosing. If you take a product that contains prebiotic fibres (e.g. inulin, FOS), be aware that these can increase gas initially—introduce gradually. Avoid products that make unsupported claims (e.g. curing disease or replacing prescription treatment). Reputable brands typically publish strain information and storage requirements; when in doubt, ask your pharmacist or dietitian for a recommendation that fits your medications and health status.
Interactions with medications
Older adults often take multiple medications. Probiotics can interact with immunosuppressants (e.g. after transplant or in autoimmune disease), and in severely immunocompromised individuals or those with central lines, live probiotics may carry a small risk of infection—such use should be discussed with a doctor. Antibiotics can reduce probiotic colonisation if taken at the same time; spacing intake (e.g. taking the probiotic two to three hours apart from the antibiotic) may improve survival of the beneficial bacteria, though evidence is mixed. Continuing the probiotic for a short period after the antibiotic course may help restore gut flora; again, discuss with your provider. There is no strong evidence that probiotics routinely interfere with most common drugs (e.g. blood pressure or diabetes medications), but because polypharmacy increases the chance of interactions, a healthcare provider or pharmacist should be consulted before starting a probiotic, especially when taking many prescriptions or when immune function is impaired. If you are on warfarin or other blood thinners, or have a history of endocarditis or valvular heart disease, your doctor may have specific guidance; document any new supplements in your medication list so all providers are aware.
Dosing and safety
Start with a low dose (e.g. 1–3 billion CFU per day) and increase gradually if well tolerated. Many studies in older adults use doses in the range of 1–10 billion CFU daily; higher doses are not necessarily more effective and may cause transient gas or discomfort. Take probiotics with a meal or as directed on the label to improve survival through the stomach. Do not use probiotics to replace prescribed treatment for infections, inflammatory bowel disease, or other conditions. If you have had recent abdominal surgery, pancreatitis, or severe acute illness, or if you are critically ill, your provider may advise against live probiotics or recommend a specific product. Report any new or worsening digestive symptoms, fever, or unusual side effects. Quality varies; choose products from reputable manufacturers that specify strain, CFU at expiry, and storage requirements.
Timing is flexible: morning with breakfast or evening with dinner are both common and acceptable unless the label specifies otherwise. Introduce one new probiotic at a time so you can tell whether it helps. When in doubt, start with one well-studied strain at a low dose. If you miss a dose, resume with the next scheduled dose; there is no need to double up. For long-term use, periodic review with your doctor or dietitian is sensible—especially if your medications or health status change—to ensure probiotics remain appropriate and are not duplicating or conflicting with other treatments.
Food and supplements
Fermented foods such as yogurt, kefir, cultured buttermilk, kimchi, sauerkraut, and some aged cheeses contain live bacteria and can contribute to dietary intake of beneficial microbes. They also provide protein, calcium, or other nutrients. For older adults with good appetite and no contraindications, including these foods regularly can support gut health alongside a fibre-rich diet and adequate fluids. Choose plain or low-sugar options when possible; added sugars can outweigh benefits for some. When appetite, chewing, swallowing, or access to a variety of foods is limited, or when a specific strain or dose is desired for a studied benefit, a supplement may be more practical. Supplements and food can be combined; there is no need to choose one or the other unless a provider advises otherwise. A dietitian can help tailor food and supplement choices to individual needs and medical history.
When to see a doctor
Do not rely on probiotics alone if you have unexplained or persistent digestive symptoms, unintended weight loss, blood in the stool, severe pain, vomiting, or a family history of digestive disease. A clinician can rule out conditions such as celiac disease, inflammatory bowel disease, malabsorption, or motility disorders. Once serious causes are excluded, a dietitian can help design a personalised diet and supplement plan. If you are already taking a probiotic and notice no improvement after 4–8 weeks, or if symptoms worsen, stop and discuss with your provider before trying another product. Red flags (e.g. fever, severe abdominal pain, or change in bowel habits that persists) warrant prompt medical evaluation regardless of supplement use. Track what you take and how you feel so you and your provider can adjust as needed.
FAQ
How long should I take a probiotic?
Many people use probiotics for 4–8 weeks to assess benefit; some continue longer under guidance. There is no universal rule—discuss duration with your provider, especially if you take multiple medications or have chronic conditions.
Can I take probiotics with antibiotics?
Yes, but spacing the probiotic a few hours from the antibiotic may improve bacterial survival. Continue the probiotic during and briefly after the antibiotic course if your doctor agrees; this may help reduce antibiotic-associated digestive upset and support recovery of the microbiome.
Are probiotics safe for seniors on many medications?
Generally yes for most common medications, but always check with your doctor or pharmacist. Special caution applies to immunosuppressants, recent surgery, central lines, or severe immune compromise—in those cases, use only with medical approval.
Key takeaways
Probiotics for seniors are best viewed as one part of a broader strategy: a fibre-rich diet, adequate fluids, regular activity where possible, and open communication with your healthcare team. When chosen with care—right strain, sensible dose, and attention to medications and safety—they can support gut and immune health in many older adults.
- Gut microbiome diversity often declines with age; diet, medications, and mobility play a role.
- Evidence supports certain probiotic strains for digestive comfort, immune support, and nutrient-related benefits in older adults, but effects are strain- and context-dependent.
- Choose products with identified strains, CFU at expiry, and evidence in ageing or senior populations when available.
- Discuss probiotics with a provider if you take multiple medications, immunosuppressants, or have had recent surgery or serious illness.
- Start with a low dose; take with food; do not replace prescribed treatment.
- Combine probiotics with fibre, fluids, and a balanced diet; use fermented foods when appropriate, and supplements when a specific strain or dose is needed.
Probiotics can be a useful part of gut and immune support for older adults when chosen with professional guidance and used as part of a balanced, evidence-based approach. Quality products from reputable brands, used as directed, offer the best chance of benefit. If you have persistent digestive symptoms, weight loss, or other red flags, see a doctor before relying on supplements alone.




