Why the Oral Microbiome Matters
Your mouth hosts a diverse community of bacteria, fungi, viruses and other microbes—the oral microbiome. Like the gut, the mouth has its own ecosystem that responds to diet, hygiene and environment. When this community is balanced, beneficial species help maintain healthy gums, support tooth enamel and keep breath fresher. An imbalance (dysbiosis) is linked to gum disease (gingivitis and periodontitis), tooth decay (cavities), bad breath (halitosis) and other oral and systemic issues. Research continues to clarify links between oral dysbiosis and conditions such as cardiovascular disease and diabetes; keeping the mouth healthy is part of overall wellness. Diet and lifestyle—including reducing sugar, avoiding tobacco and maintaining good oral hygiene—form the foundation; probiotics are one optional layer that may support the oral microbiome for some people. As a registered dietitian, I emphasise that probiotics for oral health are a complement to—not a replacement for—brushing with fluoride toothpaste, flossing and regular dental check-ups.
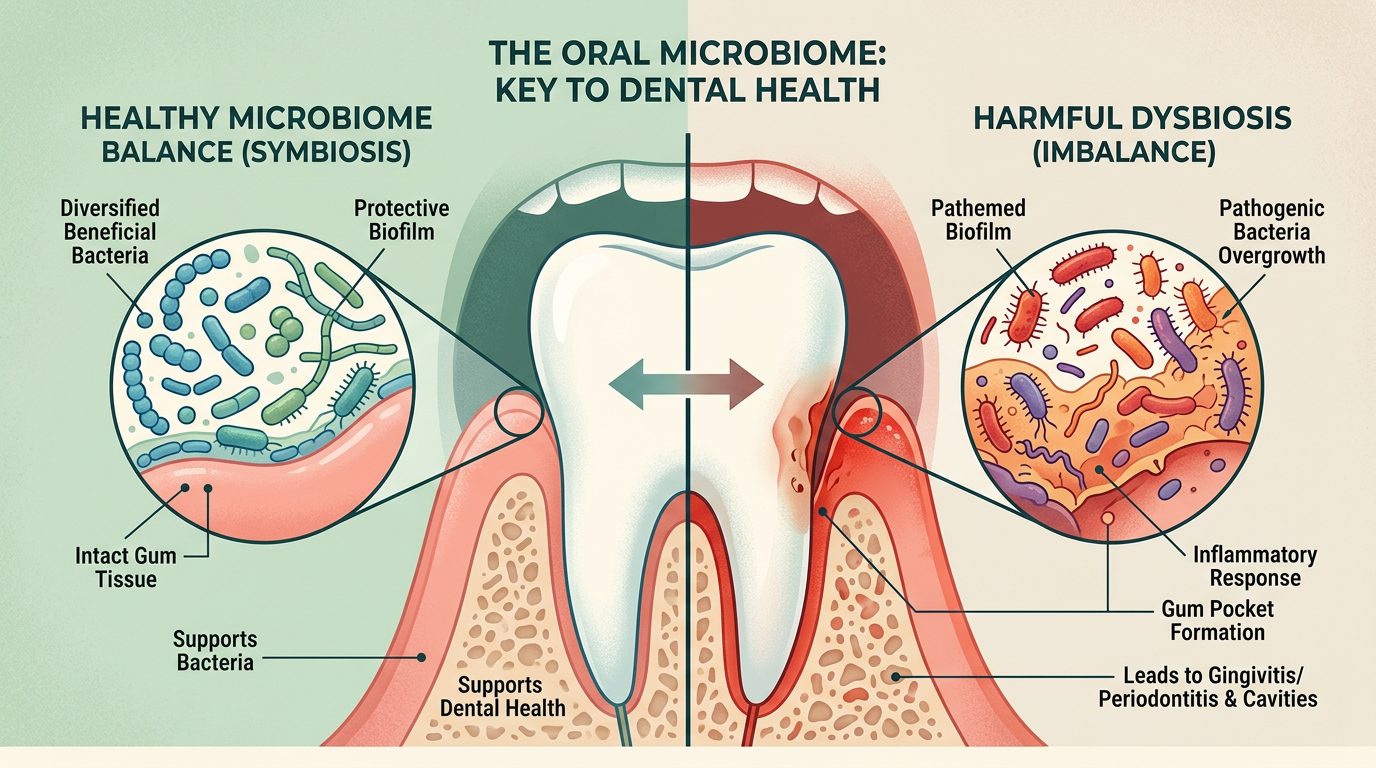
The Oral Microbiome in Brief
The oral cavity contains hundreds of species living on the tongue, gums, teeth, cheeks and palate. Different sites—tongue, gingival crevice, tooth surface—host slightly different communities. These microbes form biofilms; when the balance favours beneficial or neutral species, they can limit the overgrowth of pathogens. Beneficial bacteria may produce hydrogen peroxide, bacteriocins or other compounds that suppress cavity-causing Streptococcus mutans and gum-disease-associated bacteria such as Porphyromonas gingivalis. They also compete for space and nutrients, help maintain a more neutral pH in plaque and interact with the local immune response. Factors that disrupt balance include a high-sugar or highly acidic diet, poor brushing and flossing, smoking, dry mouth (xerostomia), antibiotics and stress. Saliva plays a key role by buffering acid, supplying minerals and helping clear food debris; conditions that reduce saliva flow can worsen dysbiosis. Probiotics are live microorganisms that, when delivered in adequate amounts to the mouth in a format that allows colonisation, may help restore or maintain a healthier balance. The goal is not to sterilise the mouth but to favour a community that supports rather than undermines oral health.
Evidence on Probiotic Strains for Oral Health
Research has focused on specific strains delivered in ways that allow them to reach oral surfaces (e.g. lozenges, chewables). Swallowed capsules are less likely to colonise the mouth because the bacteria pass through quickly and are exposed to saliva and swallowing; for oral benefit, products designed for oral use are preferred. Studies vary in design, dose and duration; not all trials show significant effects, and individual response can vary. Below is a concise, evidence-based overview of what the current literature suggests for gum health, cavities and bad breath.
Gum Health (Gingivitis and Periodontitis)
Lactobacillus reuteri (e.g. strains DSM 17938 and ATCC PTA 5289) is among the most studied for gingival health. Several randomised controlled trials (RCTs) report reductions in gingival inflammation, bleeding on probing and plaque indices when participants use L. reuteri lozenges or tablets in addition to usual hygiene, compared with placebo. Doses in trials often range from about 108 to 109 CFU per day, with treatment periods of four to twelve weeks. Lactobacillus salivarius and Lactobacillus brevis have also been studied with modest improvements in some gum health markers. Effects are generally modest and variable; not everyone responds, and probiotics do not replace treatment for active periodontitis. Combining probiotics with good brushing, flossing and professional cleanings may offer the best chance of benefit for those with mild to moderate gingivitis. Scaling, root planing and ongoing professional care remain essential for established gum disease. The mechanism is thought to involve competition for nutrients and binding sites, modulation of the immune response and possibly production of antimicrobial substances. Long-term colonisation after stopping the product is not guaranteed; some studies suggest that continued or periodic use may be needed to sustain benefits.
Cavities (Caries) and Cavity-Causing Bacteria
Streptococcus mutans is a major driver of tooth decay because it produces acid and contributes to plaque formation. When you eat or drink sugar, these bacteria ferment it and lower the pH at the tooth surface, which can lead to demineralisation and cavities over time. Probiotics that can colonise the mouth and compete with or suppress S. mutans have been investigated in children and adults. Lactobacillus reuteri, Lactobacillus paracasei, Lactobacillus rhamnosus GG and Streptococcus salivarius (e.g. strain K12) have shown reductions in S. mutans counts or caries-related outcomes in some studies. Results depend on strain, dose, format and duration; evidence is promising but not yet sufficient to claim that probiotics alone prevent cavities. They may offer a small additional benefit alongside fluoride, a diet lower in free sugars and good hygiene. Reducing frequency of sugary snacks and drinks and brushing twice daily with fluoride toothpaste remain the cornerstone of caries prevention. If you or your child are at high caries risk, your dentist can advise on fluoride varnish, sealants and diet; oral probiotics may be discussed as one possible adjunct.
Bad Breath (Halitosis)
Halitosis often stems from volatile sulphur compounds (VSCs) produced by bacteria on the tongue, in periodontal pockets and in other oral niches. The back of the tongue is a common reservoir for these bacteria, which is why tongue cleaning can help. Oral probiotics that colonise the tongue and other surfaces may reduce the abundance of odour-producing species. Streptococcus salivarius K12 produces bacteriocins that can inhibit some odour-producing species. Several trials using K12 lozenges report improvements in breath odour (organoleptic scores) and/or bacterial counts when used over several weeks. Lactobacillus salivarius and other oral probiotics have also been studied with mixed results. Consistent use over four to twelve weeks may be needed to see an effect; good oral hygiene—including tongue cleaning, flossing and regular dental visits—remains the foundation for managing bad breath. If halitosis persists despite good hygiene and oral probiotics, your dentist or doctor can help rule out other causes (e.g. sinus issues, digestive conditions, certain medications).
How to Use Oral Probiotics: Lozenges, Foods and Timing

Lozenges and Chewables
Oral-specific probiotics are often sold as lozenges or chewable tablets that dissolve or are held in the mouth. This allows bacteria to adhere to oral surfaces and exert local effects. Use according to the label: typically one or two lozenges per day, after brushing or between meals, and allow them to dissolve slowly rather than chewing and swallowing quickly. Many studies use doses in the range of 108–109 CFU per day. Store products as directed (often refrigerated or in a cool, dry place) to maintain viability. Avoid eating or drinking for a short period (e.g. 15–30 minutes) after use if the label recommends it, to give bacteria time to adhere. When choosing a product, look for one that lists the strain(s) and CFU count and is intended for oral use. Avoid opening lozenges or chewables and swallowing them like a pill—the intent is to keep the bacteria in contact with the mouth. If you are unsure which product to choose, a pharmacist or dietitian can help you match your goal (e.g. gum health, breath) to a product with the right strains.
Choosing an Oral Probiotic Product
Quality oral probiotics typically state the strain name (e.g. Lactobacillus reuteri DSM 17938) and the number of live organisms (CFU) per serving. Formats designed for oral use—lozenges, chewables or dissolvable tablets—are preferable to swallowed capsules when the aim is to support the mouth microbiome. Check the use-by date and storage instructions; many products require refrigeration to maintain viability. If you have multiple oral health concerns (e.g. gums and breath), some products combine strains such as L. reuteri and S. salivarius K12 in one formulation. Reading the label for strain names and CFU will help you compare products and choose one that matches the evidence for your goal.
Probiotic Foods and the Mouth
Fermented foods (yoghurt, kefir, fermented vegetables) provide beneficial bacteria that pass through the mouth. They are not a substitute for oral-specific products if the goal is to colonise the mouth with strains proven for oral health; swallowed bacteria are largely cleared by saliva and stomach acid and do not reliably establish in the oral cavity. That said, a diet rich in fermented foods supports overall microbiome and general health, and may contribute to a healthier oral environment when combined with good hygiene. For targeted oral benefits, use a product formulated for the mouth with evidence-based strains. Eating a balanced diet with plenty of fibre, vitamins and minerals also supports oral and systemic health; for example, vitamin C is important for gum tissue, and calcium and phosphorus support tooth structure. Probiotic foods and oral probiotics can coexist in a healthy routine—one supports general and gut health, the other targets the mouth when used in the right format.
Timing and Consistency
Taking oral probiotics after brushing or between meals can help maximise contact with oral surfaces and reduce wash-out by food or drink. Use consistently for several weeks (e.g. 4–12 weeks in many studies) before expecting noticeable changes in gum comfort, breath or dentist-assessed outcomes. Do not use probiotics in place of fluoride toothpaste or professional care. If you use mouthwash, consider timing it away from probiotic use so it does not remove the bacteria you are trying to establish. Most trials run for at least four weeks; if you are using probiotics for breath or gum comfort, give it several weeks before judging effect. Let your dentist know you are using an oral probiotic so they can factor it into your care plan. Skipping days or stopping after a week is unlikely to show much effect; consistency over at least a few weeks is what the evidence suggests.
Safety and Who Should Take Care
Oral probiotics are generally well tolerated in healthy adults. Side effects are uncommon and usually mild (e.g. transient digestive or oral discomfort). Most trials report no serious adverse events. As with any supplement, buy from a reputable source and store the product as directed to ensure viability and quality. People who are immunocompromised (e.g. on immunosuppressive therapy, with certain blood disorders or after organ transplant), have central venous catheters or serious underlying illness should consult a healthcare provider before using live probiotics. Do not give oral probiotic products to very young children without professional advice. Probiotics do not replace treatment for active gum disease, cavities or oral infections—see a dentist for diagnosis and care. If you have dentures, implants or orthodontics, maintain your usual hygiene and discuss adding oral probiotics with your dentist. Pregnant or breastfeeding women should follow the same caution as for any supplement and check with their provider if unsure. Discontinue use and seek advice if you experience persistent discomfort or signs of infection. Oral probiotics are not a treatment for acute dental problems such as abscesses or severe gum disease; those require professional diagnosis and care.
Key Takeaways
- The mouth has its own microbiome; balance supports gum health, tooth health and fresher breath.
- Strains with the most evidence for oral use include Lactobacillus reuteri, Lactobacillus salivarius and Streptococcus salivarius K12.
- Use products designed for oral use (lozenges or chewables) so bacteria can colonise the mouth; follow label directions for dose and timing.
- Take after brushing or between meals; allow lozenges to dissolve; use consistently for several weeks.
- Probiotics are an adjunct to—not a replacement for—brushing, flossing, fluoride and regular dental check-ups.
- If immunocompromised or unsure, check with your provider before use. Do not use instead of treatment for active gum disease or cavities.
Probiotics for oral health can be a useful addition to a complete dental care routine when you choose evidence-based strains, use them as intended and keep up with professional guidance. Prioritise brushing with fluoride toothpaste at least twice daily, flossing, limiting sugary foods and drinks, and seeing your dentist regularly; then consider oral probiotics as an optional extra if you want to support your mouth microbiome. Choosing strains with research behind them and using them as directed gives you the best chance of benefit. For a range of probiotic options, including oral-specific formulations, you can browse probiotics on iHerb.